Financial, Insurance
Medical Tourism – What You Should Know

Kathy Dicenso, CFP®
June 21, 2018
The latest Deloitte Center for Healthcare Solutions report on Medical Tourism projects renewed growth in medical tourism in 2010 as the economy recovers. The reasons? Consumer pocketbooks will be able to better withstand trips for non-emergency care outside the country. Also, it’s believed that more insurance companies will eventually agree to fund procedures at international hospitals that win extensive accreditation.
The consulting firm division’s 2009 report predicts that the number of people leaving the United States for various procedures will reach 1.6 million by 2012. That’s more than double 2007s numbers.
Medical tourism used to be all about cosmetic procedures — hiding the occasional face-lift or tummy tuck from prying eyes back home. But today, the rising number of underinsured or budget-conscious patients has made going abroad for medical care much more prevalent and for more complex procedures such as knee or hip replacements. It’s also getting the support of domestic insurers and the American Medical Association, which has set nine guidelines for patients and medical travel.
“Compare the cost of a qualified facility overseas to a negotiated price for treatment here – always ask if you can get the care cheaper in the U.S. first.”
But before you hop on the plane, it’s best to do significant due diligence of financial and safety issues related to the procedure and the hospital where it would be done. First, check and see if your insurer supports medical tourism and makes its own recommendations on where you might go for certain procedures. Insurers like Aetna, WellPoint and BlueCross BlueShield of South Carolina have tested foreign facilities in their physician and hospital net-works, arranging one-stop shopping for overseas treatments including care, travel and lodging for patients and their families.
But whether your insurer offers these options or not, the first step is researching the institution. The primary way to do that is to consult Joint Commission International (JCT), a division of the leading U.S. organization that reviews hospitals for quality, now provides similar services to hospitals abroad. JCI provides an online list of accredited hospitals and medical centers worldwide. (In fact, even if you aren’t planning a trip strictly for a medical procedure, the JCI list is a good one to use when planning a vacation – it will help you determine the best hospitals abroad if you need emergency care.) But learning about good overseas hospitals is just the first step. Consider the following:
Include your doctors: Don’t assume your doctors are automatically going to veto your thinking. They may help you find the right program, particularly if you’re having trouble affording procedures here at home. Compare the cost of a qualified facility overseas to a negotiated price for treatment here – always ask if you can get the care cheaper in the U.S. first. Whatever happens, the discussion shouldn’t end at where you should go for overseas treatment – if there are complications or a need for aftercare, it’s very important your doctor be involved.
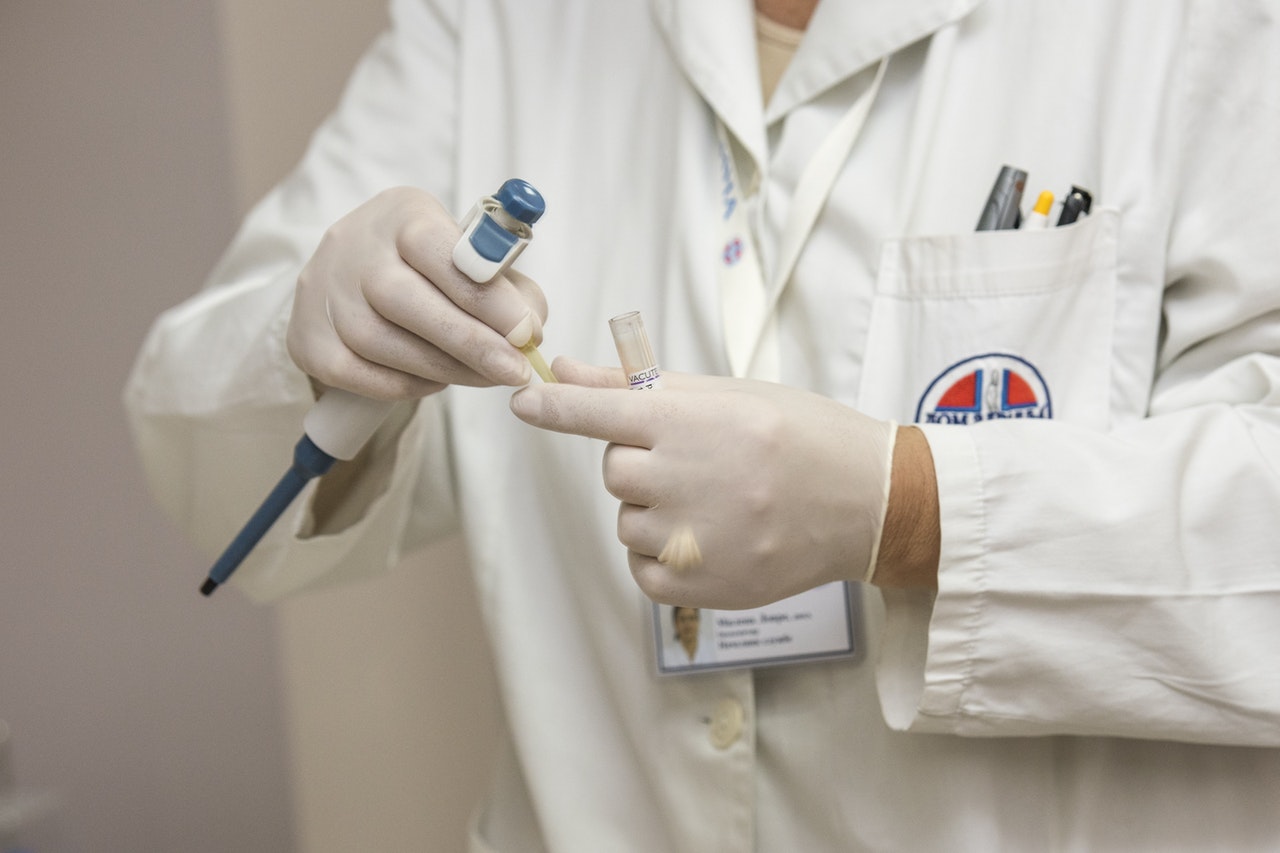
Include your doctors: Don’t assume your doctors are automatically going to veto your thinking. They may help you find the right program, particularly if you’re having trouble affording procedures here at home.
Check your employer first, then your insurer: If you are insured through your employer, start with human resources to get an overview of where your various plans stand on overseas medical coverage. Disclosure is best. If an insurer doesn’t endorse treatments at a particular hospital, it’s likely going to be tough to get them to cover any problems that could crop up domestically after overseas treatment. Ask them how – or if – they would deal with post-care complications. Also, if you have long-term care insurance, check in with them to find out if getting treatment overseas could potentially risk your coverage when you need to draw on it later.
Get some money advice: If you are planning a non-emergency procedure that won’t be covered by insurance, take the opportunity to see how such a move will affect your overall finances. It makes sense to talk to a financial advisor such as a financial planning professional to weigh this expenditure – which may still be in the tens of thousands even at a sizable discount – against your other financial needs and concerns.
Designate a family member as your primary contact: Choose a family member, with your family, friends and employers you designate they call. This primary contact should also be prepared to pay bills and deal with the unthinkable – if you suffer complications or die outside the US.
Make sure your health care directives work where you’re going: A health care directive – also called an advance directive – specifies your medical wishes in case you’re incapacitated. They come in two forms: the living will and the power of attorney for health care. The living will indicates specific wishes about medication and life-support treatment if you’re incapacitated, and you need to refer to your own state laws on how these documents need to be written.
“Get some money advice: If you are planning a non-emergency procedure that won’t be covered by insurance, take the opportunity to see how such a move will affect your overall finances.”
The power of attorney for health care – also called a durable power of attorney for health care – also specifies your wishes for treatment but allows you to designate a specific person to act in your stead if you are incapacitated. You should check with the hospital where you’ll be doing the procedure as well as your attorney about what documentation will be effective where you’re going.
Pick your representatives wisely: Your health care power of attorney may or may not be the person with the power to disburse your assets if you’re incapacitated, but that person should have their name on a joint checking account in case bills need to be paid. Also, make sure you have a line of credit established that your designated representative can access in case of emergency. Make sure all these sources of cash can flow easily to the foreign country where you’re recovering.
Update your estate matters: No one expects they’ll die in the hospital, but it’s necessary that your Will be up to date so your spouse or designated executor can step in immediately to handle your affairs. Again, it makes sense to see whether any-thing needs to be amended based on out-of-country care.
Have an up-to-date disaster plan: If you are incapacitated or die, it makes sense to have all critical papers and data in one place so your health care power of attorney, your executor or a trusted friend or family member can access them.
Kathy DiCenso, Certified Financial Planner, is President of DiCenso & Associates. She can be reached at (775) 336-0021 or kathydicenso@lpl.com.
More from DiCenso & Associates...
Want new articles before they get published?
Subscribe to our Newsletter.

At DiCenso & Associates, we use our passion and expertise in finance striving to inspire, educate, grow and secure your financial future.
Getting Started
Contact Us
Office Hours: M-F, 9am-5pm
Call Us: (775) 336-0021
Directions: Map It
Securities and Advisory services offered through LPL Financial, a Registered Investment Advisor, Member FINRA / SIPC.
The LPL Financial representatives associated with this site may only discuss and/or transact securities business with residents of the following states: AZ, CA, CO, HI, IA, ID, KS, ME, NC, NH, NM, NV, OR, SC, SD, TX, VA, and WA.
Website by Jolly Creative Agency. WebCare®
Check the background of this financial professional on FINRA’s BrokerCheck.
